Connection Makes the Difference – A Collaborative Shift in Bedside Manner?
Healthcare 2.0 is all about connecting. Take your pick: you can communicate via blogs, tweets, IMs, wikis, or social networks. And then, of course, you can opt for just plain old face-to-face dialogue.
The Communication Explosion
According to ME-P experts and Business of Medical Practice textbook contributors Mario Moussa PhD and Jennifer Tomasik MA, on the face of it, the explosion of communication options seems like a very good thing indeed.
www.BusinessofMedicalPractice.com
In the most basic ways, human beings need connection. Without the give and take of social interaction, our health suffers. In extreme situations—in solitary confinement or similar conditions—the brain almost completely shuts down.
What We Can Learn from Terry Anderson
The journalist Terry Anderson was held hostage in Lebanon from 1985 to 1992, enduring months at a time of almost complete isolation. In his memoir Den of Lions, Anderson described the catastrophic result: “The mind is a blank…. Where are all the things I learned, the books I read, the poems I memorized? There’s nothing there, just a formless, gray-black misery. My mind’s gone dead.”
The Link Between Social Connection and Good Health
On the positive side, studies have established a link between social connection and good health. (Even contact with people you dislike is better than having no contact at all). The same goes for the relationship between doctor and patient: data show that when the relationship is satisfying, it has tangible health benefits.
For example, when patients have a positive emotional connection with their doctors, they remember a higher percentage of care-related information and even experience significantly better physiological outcomes.
The Conversation
And the way doctors converse with patients—apart from the actual content of the conversations—has an equally powerful effect:
Do you want your patient’s nagging headaches to go away?
Discuss their expectations and feelings, in addition to the neurological facts. This is much more effective than sticking to the facts alone, since a strong psychological bond is strong medicine.
Do you want your medical advice to be followed?
Draw your patient into conversations about treatment. The research shows that engagement makes a difference.
Assessment
Is there an analogy here for financial advisors and medical management consultants?
Conclusion
Your thoughts and comments on this ME-P are appreciated. Feel free to review our top-left column, and top-right sidebar materials, links, URLs and related websites, too. Then, subscribe to the ME-P. It is fast, free and secure.
Speaker: If you need a moderator or speaker for an upcoming event, Dr. David E. Marcinko; MBA – Publisher-in-Chief of the Medical Executive-Post – is available for seminar or speaking engagements. Contact: MarcinkoAdvisors@msn.com
OUR OTHER PRINT BOOKS AND RELATED INFORMATION SOURCES:
- PRACTICES: www.BusinessofMedicalPractice.com
- HOSPITALS: http://www.crcpress.com/product/isbn/9781466558731
- CLINICS: http://www.crcpress.com/product/isbn/9781439879900
- ADVISORS: www.CertifiedMedicalPlanner.org
- FINANCE: Financial Planning for Physicians and Advisors
- INSURANCE: Risk Management and Insurance Strategies for Physicians and Advisors
- Dictionary of Health Economics and Finance
- Dictionary of Health Information Technology and Security
- Dictionary of Health Insurance and Managed Care
Filed under: Book Reviews, Information Technology, Practice Management, Quality Initiatives | Tagged: Business of Medical Practice, Jennifer Tomasik, Mario Moussa, Patient Experience, social media in medicine, www.BusinessofMedicalPractice.com |
















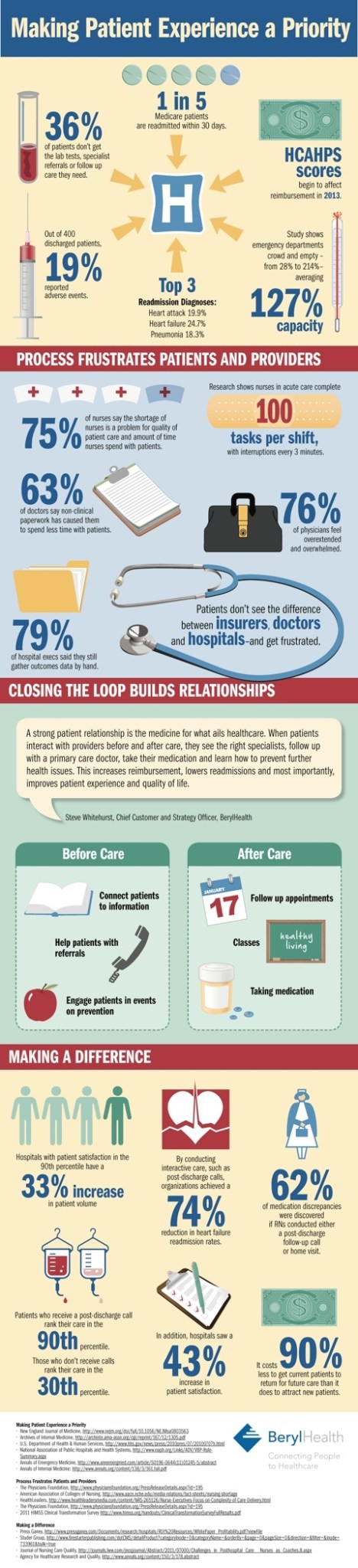

The “Patient Experience”
Back in the day the patient experience was known as bedside manner.
Susan
LikeLike
Patients Want Texts and Emails from Docs
A new survey finds that patients’ expectations for healthcare providers have evolved. A majority expect their doctors to communicate with them proactively – even when they’re well – via texts, emails and proactive smartphone alerts.
http://www.healthcareitnews.com/news/patients-want-texts-and-emails-sickness-and-health
For example, nearly 80 percent of respondents say it’s their doctor’s job to keep them healthy – not just to treat them when they’re sick. And, they wish there was more communication when they’re feeling OK.
Call this e-bedside manner, if you will.
Hope Rachel Hetico RN MHA
LikeLike
Patient Engagement
Today, requirements and regulations are leading us on a path where physician reimbursement could be based on outcomes.
Combine that fact with the issue of outpatient overtaking inpatient, and engaging patients in their own care becomes crucial.
http://www.physbiztech.com/how-to/critical-communications-five-ways-improve-patient-engagement?email=MARCINKOADVISORS@MSN.COM&GroupID=116654
So, here are five key rules to follow to improve that dynamic exchange.
Dr. Renuka
LikeLike
Bettering the Patient Experience
In this essay, Marty Stempniak asks what is the next big thing in patient experience? Are flat-screen TVs and comfy furniture in hospital rooms the answer? Or should providers pursue a simpler, more human solution?
http://www.hhnmag.com/hhnmag/HHNDaily/HHNDailyDisplay.dhtml?id=3590002086
ME-P Readers, please have your say.
Ann Miller RN MHA
LikeLike
On P4 Medicine
According to MOLLY MALOOF MD, the healthcare industry is changing as new models of care and reimbursement emerge. One of these approaches is P4 Medicine. P4 Medicine stands for predictive, preventive, personalized, and participatory. In my opinion, P4 Medicine is one of the best models for maximizing patient engagement.
The earliest manifestation of P4 Medicine began eight years ago at the Institute of Systems Biology when Dr. Lee Hood MD PhD, a physician scientist and creator of the automated gene sequencer, recognized that the application of systems biology to medicine would fundamentally alter our understanding of health and disease.
This model has merged three powerful aspects of science and technology:
1. Systems biology (defined as the study of biological systems as collections of networks at multiple levels, ranging from the molecular level, through cells, tissues and organisms, to the population level)
2. The digital revolution (e.g., big data and analytics, wearable technology, mobile technology, etc.)
3. Consumer-driven healthcare (e.g., patient/consumer activated social networks).
http://thehealthcareblog.com/blog/2015/09/23/how-i-use-p4-medicine-to-maximize-patient-engagement/
Any devotees or thoughts?
Dr. May
LikeLike